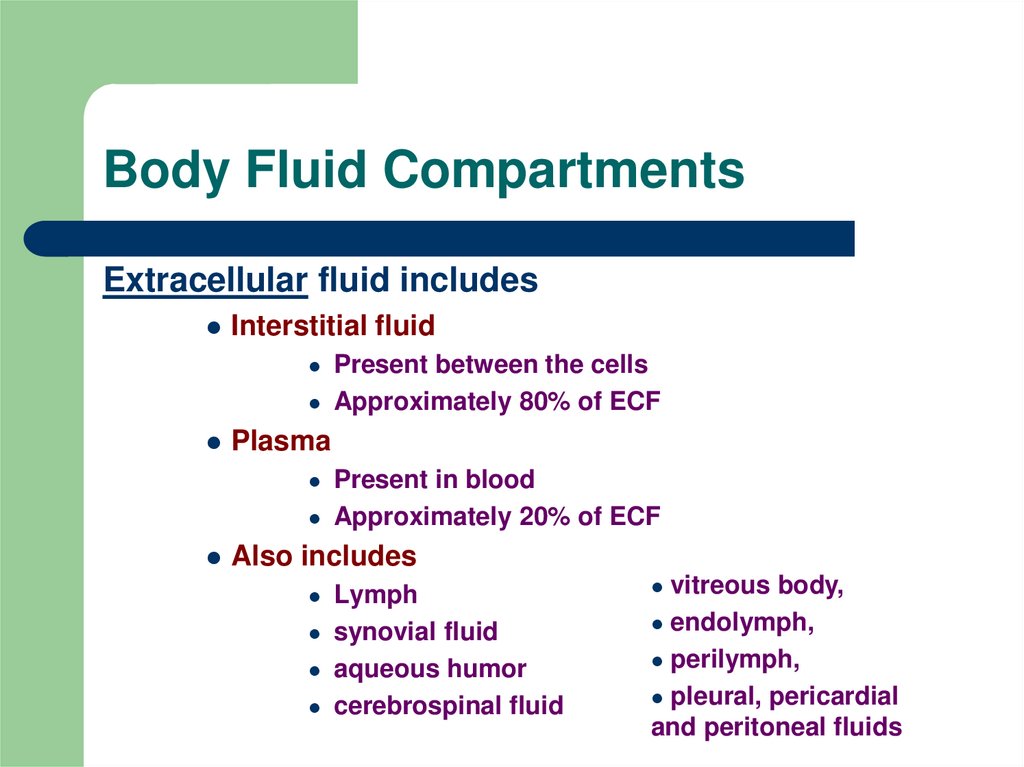
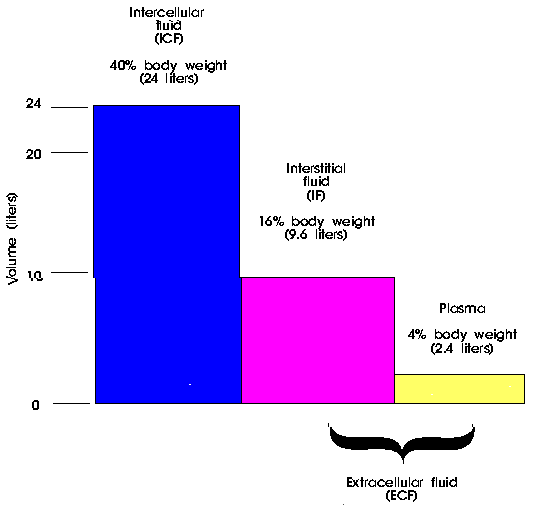
Review intracellular extracellular body fluid compartments
The greatest effect is in patients with temporary albumin loss, for example trauma, surgery or burns (Kokko and Tannen, 1996). Albumin replacement colloid therapy is indicated for hypoalbuminaemia volume-depleted patients. A reduction in albumin due to loss, for example in sepsis where there is a higher rate of albumin loss into the tissues, may result in hypotension and hypovolaemia (Kokko and Tannen, 1996). The protein assists in maintaining colloid osmotic pressure in the circulation (approximately 70-80% of osmotic pressure is created by albumin). Colloid solutions are not generally indicated for most patients for ECF replacement (RCUK, 2005 Nolan, 2001 Smith, 2000) because they move easily into the ICF making them less effective and creating other clinical issues (for example pulmonary oedema and hypotension).Īlbumin levels are also important in fluid balance, and should be monitored closely. In general crystalloid fluids (for example saline 0.9% solution or Hartmann’s solution) are recommended as they remain in the ECF longer and are isotonic - that is, they match blood tonicity (Docherty and McIntyre, 2002 RCUK, 2000). In some cases patients will need fluid and electrolyte replacement therapy, which nurses are responsible for delivering and monitoring. Daily input and output is summarised in Table 1. The average fluid input per day is 2,500ml (water as food 1,000ml, water as liquid 1,200ml, water from catabolism 300ml) and output is 2,500ml. These figures may differ slightly according to local policies. The serum sodium level defined as ‘normal’ is 135-145mg/dl the normal potassium level is 3.5-4.5mg/dl and the normal magnesium level is 0.6-1.0mg/dl (Metheny, 1996). For example, cardiac arrhythmias are triggered by low potassium and low magnesium levels (Docherty, 2002 Smith, 2000). If there is too much or too little of any of these electrolytes this can cause problems.

In addition, ‘ electrolyte balance’ is essential, in other words the correct concentration of various ions in the body, namely sodium, potassium and magnesium. To attain the correct balance of ECF and ICF a patient must also take in the correct amount of fluid (Docherty and McIntyre, 2002).
Regulation of ECF osmolarity is achieved by balancing the intake and output of sodium with that of water. In addition to regulating total volume, the osmolarity of bodily fluids is closely monitored and regulated because variations may cause damage to cellular structure (swelling or shrinking), disrupting normal cellular function (Edwards, 2001 Metheny, 1996). These receptors trigger ADH release, thus conserving water at the kidneys (Tortora and Grabowski, 2002 Metheny, 1996). The aorta and carotid arteries also have receptors that are sensitive to a reduction in blood pressure (related to the pressure in the left ventricle). They stop ADH secretion, which leads to increased excretion of water through renal filtration. Sensors detect stretching of the atria of the heart indicating excessive returning volume of ECF (increased venous return). Normal levels of sodium in the ECF will attract and maintain the optimum amount of water (Tortora and Grabowski, 2002 Edwards, 2001).ĪDH release is also influenced in the following circumstances.
When sodium concentration in the blood decreases the adrenal cortex is stimulated into secreting the hormone aldosterone, which instructs the distal nephrons of the kidney to retain more sodium. This in turn results in more concentrated urine and an increase in water returned to the ECF, thus correcting the volume depletion (Tortora and Grabowski, 2002 Edwards, 2001) (Fig 1). In response, the posterior pituitary gland releases antidiuretic hormone (ADH, sometimes called vasopressin) into the bloodstream, resulting in the kidneys retaining water. The hypothalamus is an osmoreceptor - a sensory end organ that reacts to changes in osmotic pressure and has an effect on the pituitary gland. When fluid volume decreases, the concentration of sodium in the blood will increase (increased osmolarity, the amount of solute per unit volume), which in turn stimulates the hypothalamus (Tortora and Grabowski, 2002). Carriage of waste products to the appropriate organ for excretion - generally through the liver and renal system.
